
‘I think we’ll carry on with what we’re doing,’ said my consultant, for what felt like the hundredth time, in January.
And yet again, I felt conflicted – because I have cancer, and what we are ‘doing’ is nothing.
I am living with several tumours in my liver and spine – but because these tumours are very small (‘sub-centimetre’) and my cancer is grade 1, which means it’s slow-growing, there is no treatment currently recommended for me.
So, at the moment, I have to live with these cancerous tumours.
I see my consultant every four months; and I always have mixed feelings when I’m told I won’t be receiving treatment.
On one hand, it’s the best news; nobody wants to hear that their tumours are growing.
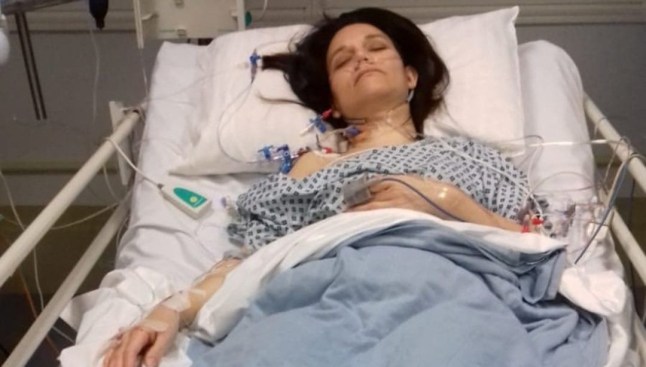
On the other hand, the cancer makes me so fatigued I can’t live a normal life – and it’s really hard knowing we’re allowing it to creep steadily forward while my quality of life slowly worsens.
I was diagnosed with a small bowel neuroendocrine tumour in 2012, age 37. The neuroendocrine system is made up of nerve and gland cells spread throughout the body; neuroendocrine cancer can grow in any of them.
It took 15 months to get diagnosed.
My first symptom, when I was 36, was a persistent cough which was misdiagnosed by my then-GP as rhinitis, post-nasal drip, asthma and reflux.
I then became very fatigued when I returned to work full-time after my youngest started school.
A blood test showed I was anaemic – but I was told by my then-GP that it was normal; I was just a ‘tired and overworked mother’.
In the six months leading up to my diagnosis, I was getting severe bloating.
I was diagnosed with IBS by that same GP and given mebeverine, a medication that relaxes muscles in the gut – but my symptoms kept getting worse.
When I asked why the mebeverine wasn’t working, my GP specifically told me: ‘You don’t have cancer’. I think she assumed that was what I was getting at. She also told me I didn’t have any symptoms that were ‘red flags’.
As I left the surgery that day, I felt she was fed up with me – but I couldn’t give up. I knew something was very wrong.
Physically, I was exhausted. In hindsight, I don’t know how I managed to carry on.
It was only when my GP went on maternity leave and I was seen by a locum doctor in November 2011 that everything changed.
This doctor looked back over my record, recognised straight away that something was wrong, and referred me to a gastroenterologist.
The gastroenterologist thought my symptoms were probably caused by constipation, but – I think because I was so desperate – he suggested the ultrasound to reassure me.
But the ultrasound found an enlarged lymph node. This discovery led to an MRI.
When the phone rang a few days later, I knew it was my MRI results; and I knew it was serious. They initially just said I needed to come in for a colonoscopy, but when I pressed them, they confirmed a mass had been seen.
In fact, the colonoscopy showed my tumour had caused an almost total bowel obstruction.
At my follow-up appointment, the doctor’s first words were, ‘I’m afraid it is cancer’. It was stage 3, meaning it had spread to the local tissues and lymph nodes.

I was really shocked. In fact, I was so lightheaded, I asked to lie down.
I had major abdominal surgery to remove the tumour, as well as sections of my small and large intestines, surrounding tissue, lymph nodes and appendix.
It was a long recovery period, but I did get better – and life more or less returned to normal. I had some digestive issues but they were manageable with medication.
I was scanned every six months for the first five years, and then yearly. But at my first yearly scan in 2019, cancer was discovered to have spread to my liver; and I was later diagnosed with incurable stage 4 cancer in 2019.
I had further major surgery to remove the cancer in my liver, but it recurred – again in my liver – in 2021. Then, one area of my spine lit up on my yearly full body PET scan in January 2024 and an MRI in March 2024 confirmed two separate lesions in my spine.
My PET scan in November 2025 lit up several areas in my spine – two of which are now confirmed metastases, the others are smaller lesions which are not yet confirmed metastases.
Neuroendocrine Cancer UK
Kerie Ivory receives support from Neuroendocrine Cancer UK (NCUK) as part of her ongoing care.
My consultant has always said that the best treatment is to simply remove the cancer. But I wasn’t able to have further liver surgery as the tumour was in an awkward place, so I was referred for radiotherapy instead.
Sadly, the radiotherapy was only partially successful, shaving just a tiny amount off the tumour.
Several other treatment options were explored but ruled out. I was turned down for alcohol ablation, for example, where they inject pure alcohol into the tumour to destroy the cancer cells, because the tumour was too small to see clearly enough for the ultrasound scan to guide the needle into the tumour.
Psychologically, it’s really hard knowing that we aren’t doing anything to stop the cancer growing.
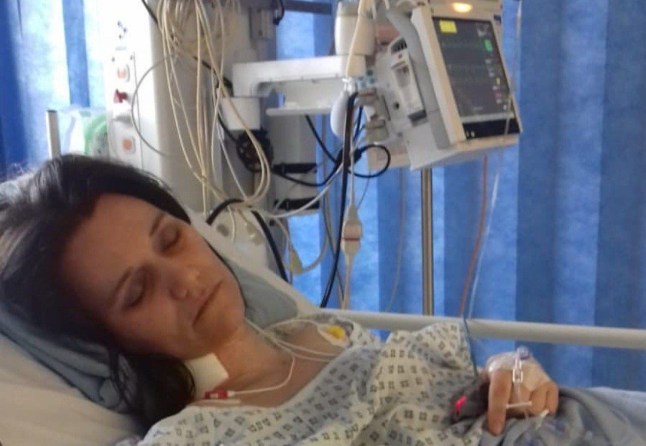
One of the worst things is fatigue. I miss the normal everyday things I took for granted when I was well, like going for a run or cooking for my family. I’ve also had to give up work.
I always dealt with anxiety by keeping busy – something I cannot do now with my fatigue – so I also struggle with my mental health. Counselling, medication and connecting with other people with incurable cancer helps enormously, but it’s hard.
I’ve always been a positive person, though. This experience has given me an even greater appreciation of all I have, and I am stronger and more resilient than ever.
I know, one day, there will be another appointment when I’m told the cancer has progressed and further treatment is recommended.
I just don’t know when that will be.
Do you have a story you’d like to share? Get in touch by emailing Ross.Mccafferty@metro.co.uk.
Share your views in the comments below.
Write Reviews
Leave a Comment
No Comments & Reviews